Peanut Allergy Explained: Symptoms, Tests, and Effective Treatments
Food Allergies
Peanut allergies are increasingly common, and understanding their symptoms, tests, and effective treatments is essential for those affected. Explore vital insights here.

Jump to a section
Peanut Allergy Explained: Symptoms, Tests, and Effective Treatments
Understanding Peanut Allergy: An Overview
Peanut allergy is a medical condition that has been increasingly prevalent, particularly in the last few decades. It is a type of food allergy that occurs when the body's immune system mistakenly identifies proteins in peanuts as harmful. This triggers an immune response, which can range from mild to severe and can affect various parts of the body. The exact cause of peanut allergies is not completely understood, but it is believed to involve a combination of genetic and environmental factors. Family history of allergies, exposure to peanuts at a young age, and certain genetic markers are considered risk factors.
In the context of food allergies, peanut allergies are particularly concerning due to their potential severity. Unlike some other food allergies, which might cause mild symptoms such as itching or gastrointestinal discomfort, peanut allergies can lead to life-threatening reactions. This makes proper diagnosis, management, and treatment crucial for those affected. The prevalence of peanut allergies has also led to increased awareness and changes in food labeling laws, aiming to protect those with the condition.
The immune response involved in peanut allergies is typically mediated by Immunoglobulin E (IgE) antibodies. Upon exposure to peanut proteins, these antibodies trigger the release of histamines and other chemicals from mast cells and basophils, leading to the symptoms associated with the allergy. Understanding the mechanisms behind peanut allergies is key to developing effective treatments and management strategies. At NYFA under Dr. Shah's leadership, we continue to evolve proper diagnosis and best possible long term freedom options with evolving science and data.

Common Symptoms of Peanut Allergy
Peanut allergies can manifest through a variety of symptoms, which can appear within minutes to hours after exposure to peanuts. These symptoms can affect different parts of the body, including the skin, gastrointestinal tract, respiratory system, and cardiovascular system. Recognizing these symptoms is essential for prompt treatment and management.
Skin reactions are among the most common symptoms of peanut allergy. These can include hives, which are red, itchy welts that appear on the skin. Eczema, a chronic skin condition characterized by itchy, inflamed patches, can also be exacerbated by peanut exposure. Swelling of the face, lips, and tongue is another common symptom, which can be particularly concerning if it affects the airway.
Gastrointestinal symptoms are also frequently observed in those with peanut allergies. These can range from mild discomfort to more severe reactions, including nausea, vomiting, and diarrhea. Abdominal pain and cramping can also occur, making it challenging to differentiate from other gastrointestinal conditions without proper diagnosis.
Respiratory symptoms can be particularly dangerous, as they can affect breathing. These symptoms include nasal congestion, runny nose, and sneezing. More severe respiratory reactions can involve coughing, wheezing, and shortness of breath. In some cases, exposure to peanuts can trigger asthma attacks in individuals with pre-existing asthma. Cardiovascular symptoms, though less common, can include dizziness, lightheadedness, and in severe cases, a drop in blood pressure, which can lead to anaphylactic shock.
Severe Reactions: Anaphylaxis Explained
Anaphylaxis is a severe, potentially life-threatening allergic reaction that can occur in individuals with peanut allergies. This reaction involves multiple organ systems and can escalate rapidly, requiring immediate medical attention. Understanding the signs and symptoms of anaphylaxis is crucial for prompt intervention and treatment.
The onset of anaphylaxis can be sudden, with symptoms appearing within minutes of exposure to peanuts. Early signs may include a feeling of warmth, tingling in the extremities, or a sense of impending doom. Skin reactions, such as hives or itching, are common initial symptoms. Swelling of the face, lips, and tongue can also occur, potentially leading to difficulty breathing.
As anaphylaxis progresses, respiratory symptoms become more pronounced. These can include swelling of the throat, which can obstruct the airway and lead to difficulty swallowing and breathing. Wheezing, shortness of breath, and chest tightness are also common. In severe cases, anaphylaxis can cause a drop in blood pressure, leading to dizziness, fainting, and shock. Gastrointestinal symptoms, such as nausea, vomiting, and diarrhea, may also be present.
Immediate treatment of anaphylaxis is critical and typically involves the administration of epinephrine, a medication that can rapidly reverse the symptoms. Epinephrine is usually administered via an auto-injector or as a nose spray, which individuals with known peanut allergies are advised to carry at all times. After administering epinephrine, it is essential to seek emergency medical care, as further treatment and monitoring may be necessary. Understanding anaphylaxis and its management is vital for individuals with peanut allergies and their caregivers.
Diagnosing Peanut Allergy: Tests and Procedures
Diagnosing a peanut allergy involves a combination of medical history, physical examination, and diagnostic tests. Accurate diagnosis is crucial for effective management and treatment, as it helps differentiate peanut allergy from other food-related conditions and ensures appropriate interventions.
The first step in diagnosing a peanut allergy is a thorough medical history and physical examination. The healthcare provider will ask about the individual's symptoms, their onset, and any potential triggers. A family history of allergies, eczema, or asthma may also be relevant, as these conditions can increase the likelihood of a peanut allergy. The physical examination may involve checking for signs of allergic reactions, such as skin rashes or respiratory symptoms.
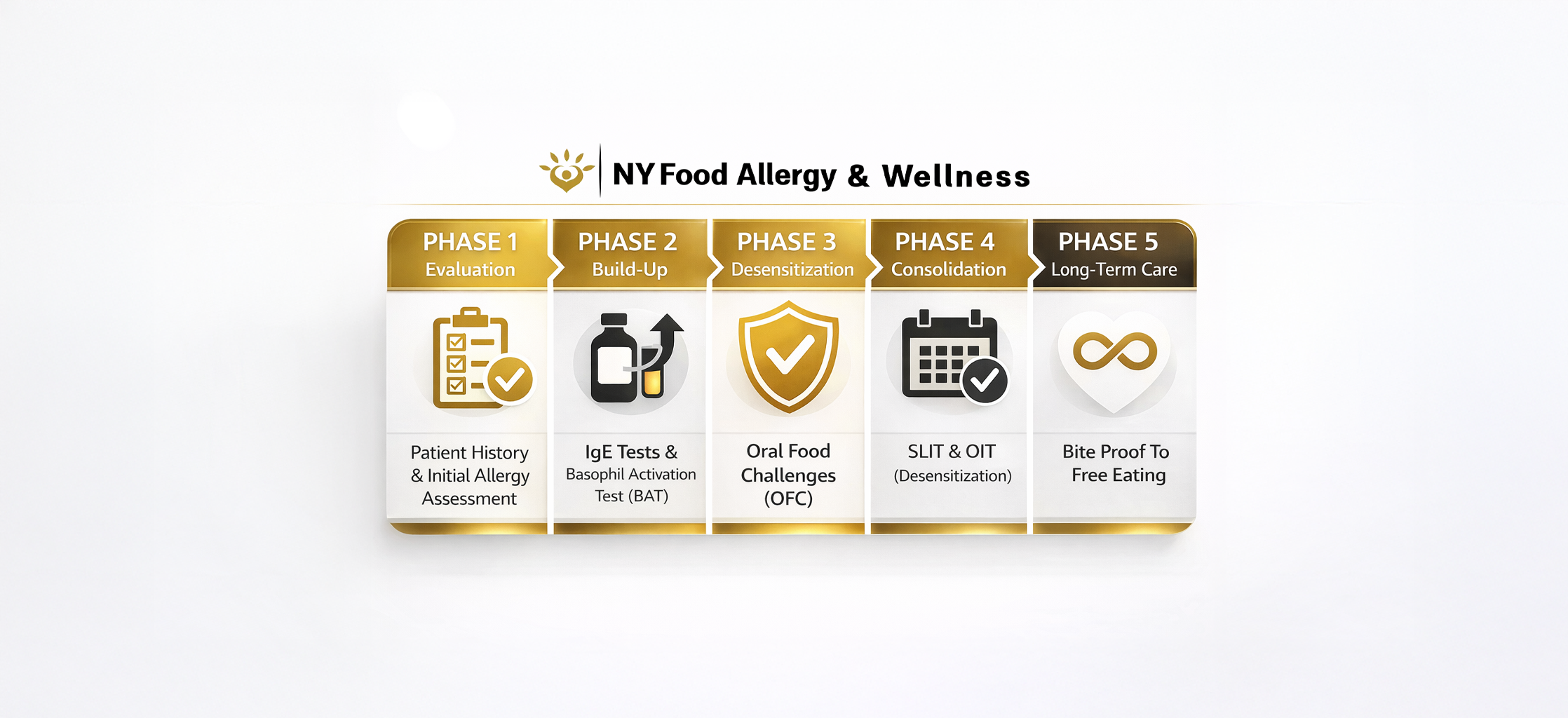
Several diagnostic tests can help confirm a peanut allergy. One of the most common tests is the skin prick test, which involves applying a small amount of peanut protein to the skin and then pricking the skin with a needle. If the individual is allergic to peanuts, a raised, red, itchy bump will appear at the test site within 15-20 minutes. Another diagnostic test is the blood test, which measures the levels of IgE antibodies specific to peanuts in the blood. Elevated levels of these antibodies can indicate an allergy. At NYFA, we offer IgE peanut component tests (Ara h 2, 6) and Basophil Activation Tests (BAT) to increase the accuracy of the peanut allergy diagnosis and to increase the safety of Oral Food Challenges. We believe that these are some of the essential steps to avoid unnecessary treatments in many patients who have been previously labeled peanut allergic by skin tests or regular blood tests.
In some cases, an oral food challenge may be necessary to confirm the diagnosis. This procedure involves the supervised ingestion of small amounts of peanut under medical supervision, with careful monitoring for any allergic reactions. While this test carries some risk, it can provide definitive evidence of a peanut allergy. The results of these tests, along with the medical history and physical examination findings, help healthcare providers make an accurate diagnosis and develop an appropriate management plan. The Basophil Activation Tests (BAT) done exclusively at NYFA can help reduce the risk of reactions during Oral Food Challenges.
Differentiating Peanut Allergy from Other Allergies
Differentiating a peanut allergy from other food allergies and allergic conditions is essential for accurate diagnosis and management. Various factors can contribute to this differentiation, including the specific symptoms, timing of reactions, and diagnostic test results. Understanding these distinctions can help ensure appropriate treatment and avoid unnecessary dietary restrictions.
One key factor in differentiating peanut allergy from other food allergies is the specific symptoms and their timing. While many food allergies can cause similar symptoms, such as hives, gastrointestinal discomfort, and respiratory issues, the severity and rapid onset of symptoms can vary. Peanut allergies are often associated with more severe reactions, including anaphylaxis, which can occur within minutes of exposure. In contrast, some other food allergies may cause delayed reactions or milder symptoms.
Diagnostic tests also play a crucial role in differentiating peanut allergy from other allergies. The skin prick test and blood test for peanut-specific IgE antibodies can help confirm the presence of a peanut allergy. However, cross-reactivity between different allergens can sometimes complicate the interpretation of these tests. For example, individuals with tree nut allergies may also test positive for peanut allergies due to similar protein structures. In such cases, an oral food challenge may be necessary to confirm the specific allergy.
The additional tests done at NYFA for IgE peanut and tree nut component and Basophil Activation Tests (BAT) helps us with an accurate diagnosis of the peanut allergy alone, combine tree nut allergy or just pollen allergy that shows up as peanut sensitivity. We believe that these are some of the essential steps to avoid unnecessary treatments in many patients who have been previously labeled peanut and tree nut allergic elsewhere.
Another important consideration is the individual's medical history and potential exposure to other allergens. A detailed history of symptoms, including the timing and context of reactions, can provide valuable clues. For example, if symptoms consistently occur after consuming peanuts but not other foods, it suggests a peanut allergy. Additionally, a history of other allergic conditions, such as eczema or asthma, can increase the likelihood of a peanut allergy. By considering these factors and conducting appropriate tests, healthcare providers can accurately differentiate peanut allergy from other allergies and develop an effective management plan.
Effective Treatments for Peanut Allergy
While conventional belief is that there is no cure for peanut allergy, at NYFA, we take a different approach. We have several effective treatments and management strategies that can help reduce the risk of severe reactions and improve the quality of life for those affected. These treatments focus on preventing exposure to peanuts, managing symptoms, and preparing for emergencies. The FATE™ Program allows not only reduce the risk of reactions but allows introducing peanuts in the diet.
The cornerstone of peanut allergy management is strict avoidance of peanuts and peanut-containing products. This requires careful reading of food labels, as peanuts can be found in various processed foods and may be listed under different names. Individuals with peanut allergies should also be cautious when dining out, as cross-contamination in restaurants can pose a significant risk. Educating friends, family, and caregivers about the allergy and the importance of avoiding peanuts is also essential. After completing the FATE™ Program, majority of our patients do not need to do these steps of avoidance.
In the event of accidental exposure, quick and effective treatment is crucial. Antihistamines can help manage mild symptoms, such as itching and hives. However, for severe reactions, including anaphylaxis, the prompt administration of epinephrine is vital. Epinephrine auto-injectors, or epinephrine nasal spray, should be carried at all times by individuals with peanut allergies and used immediately if symptoms of anaphylaxis occur. After administering epinephrine, it is important to seek emergency medical care, as further treatment and monitoring may be necessary.
For some individuals, allergen immunotherapy, also known as desensitization, may be an option. This treatment involves gradually exposing the individual to increasing amounts of peanut protein under medical supervision to build tolerance and reduce the severity of allergic reactions. While not suitable for everyone, immunotherapy has shown promise in most cases and can significantly improve the quality of life. Working closely with an allergist or immunologist to develop a personalized treatment plan is essential for effectively managing peanut allergy.
Through our FATE™ Program at NYFA, we offer Sublingual Immunotherapy (SLIT) and Oral Immunotherapy (OIT) with or without biologics for infants, children, adolescents and adults. We allow patients and families to choose "bite-proof" protection to free-eating goals. We combine multiple foods to expedite the process and freedom.
Managing Peanut Allergy in Daily Life
Living with a peanut allergy requires constant vigilance and proactive management to reduce the risk of accidental exposure and ensure prompt treatment of any allergic reactions. By implementing practical strategies and educating those around them, individuals with peanut allergies can lead safe and fulfilling lives.
One of the most important aspects of managing peanut allergy in daily life is careful reading of food labels. Peanuts can be found in a wide range of foods, including baked goods, candies, and processed snacks. Additionally, peanuts may be listed under different names, such as groundnuts or arachis oil. Familiarizing oneself with these names and thoroughly checking ingredient lists can help avoid accidental exposure. When in doubt, contacting the manufacturer for clarification can provide additional peace of mind.
Dining out can be particularly challenging for those with peanut allergies due to the risk of cross-contamination. It is important to inform restaurant staff about the allergy and ask detailed questions about the ingredients and preparation methods. Some restaurants may have dedicated allergen-free areas or protocols in place to reduce the risk of cross-contact. Additionally, carrying a chef card that outlines the allergy and necessary precautions can be helpful when communicating with restaurant staff.
Educating friends, family, and caregivers about the peanut allergy and its management is essential. This includes teaching them how to recognize the signs of an allergic reaction and how to administer epinephrine in case of an emergency. Schools, workplaces, and other environments should also be informed about the allergy and any necessary precautions. By creating a supportive network and implementing proactive measures, individuals with peanut allergies can effectively manage their condition and reduce the risk of severe reactions.
The Role of Immunotherapy in Peanut Allergy Treatment
Immunotherapy, also known as desensitization, is a well-established recommended treatment at NYFA for peanut allergy that reduces the severity of allergic reactions and improves the quality of life for those affected. This treatment involves gradually exposing the individual to increasing amounts of peanut protein under medical supervision to build tolerance and reduce sensitivity.
The goal of immunotherapy is to increase the threshold at which an allergic reaction occurs. This means that individuals who undergo successful immunotherapy may be able to tolerate small and large amounts of peanuts without experiencing allergic reactions. This can significantly reduce the risk of accidental exposure and provide greater peace of mind in daily life. Our FATE™ Program simply means Food Allergy Tolerance Enhancement Program and allows patients to reach the quality of life they truly deserve.
Immunotherapy for peanut allergy can be administered in several forms, including oral immunotherapy (OIT), sublingual immunotherapy (SLIT), and epicutaneous immunotherapy (EPIT). Oral immunotherapy involves ingesting small, gradually increasing doses of peanut protein, while sublingual immunotherapy involves placing the allergen under the tongue. Epicutaneous immunotherapy, also known as the peanut patch, involves wearing a patch that releases small amounts of peanut protein through the skin. Each method has its advantages and potential risks, and the choice of treatment depends on the individual's specific circumstances and preferences.
While immunotherapy is very effective, it is not suitable for everyone and carries some risks, including the potential for severe allergic reactions during treatment. Therefore, it is essential to undergo immunotherapy under the supervision of a qualified allergist or immunologist. It is equally important to get the accurate diagnosis of peanut allergy so that you do not start any form of immunotherapy when you may not have a true peanut allergy. At New York Food Allergy & Wellness (NYFA), we devote time and technology for accurate diagnosis with IgE component tests, BAT and oral challenges. Those who need immunotherapy, we have options of food SLIT and OIT for single and multiple foods to reach your safety goals or food freedom.
Latest Research and Developments in Peanut Allergy
The field of peanut allergy research is rapidly evolving, with ongoing studies exploring new treatments, preventive measures, and potential cures. These advancements hold the promise of improving the quality of life for those with peanut allergies and reducing the burden of this condition.
One area of active research is the development of new immunotherapy approaches. While traditional immunotherapy methods, such as oral immunotherapy, have shown promise, researchers are investigating alternative methods to improve safety and efficacy. For example, researchers are exploring the use of biologics, which are medications that target specific components of the immune system, to enhance the effectiveness of immunotherapy and reduce the risk of adverse reactions. Additionally, combination therapies that include both immunotherapy and biologics are being studied to determine their potential benefits.
Another promising area of research is the investigation of early introduction of peanuts in infants to prevent the development of peanut allergies. Studies have shown that introducing peanuts to infants at high risk of developing allergies, such as those with severe eczema or egg allergy, can significantly reduce the risk of developing a peanut allergy. This has led to changes in guidelines for introducing allergenic foods to infants, with the goal of reducing the prevalence of peanut allergies in future generations.
Researchers are also exploring the genetic and environmental factors that contribute to the development of peanut allergies. Understanding these factors can help identify individuals at risk and inform preventive strategies. For example, studies are investigating the role of the gut microbiome in the development of allergies and whether modifying the microbiome through diet or probiotics can reduce the risk of peanut allergies. As research in this field continues to advance, there is hope for new treatments and preventive measures that can significantly impact the lives of those with peanut allergies.
Conclusion: Living with Peanut Allergy
Living with a peanut allergy presents unique challenges, but with proper management and support, individuals with this condition can lead safe and fulfilling lives. Understanding the symptoms, undergoing accurate diagnosis, and implementing effective treatments are key components of managing peanut allergies. Additionally, staying informed about the latest research and developments can provide hope for new treatments and improved outcomes.
Education and awareness are crucial in managing peanut allergies. By educating themselves and those around them about the allergy, individuals can reduce the risk of accidental exposure and ensure prompt treatment in case of an allergic reaction. Carrying epinephrine auto-injectors, reading food labels carefully, and communicating with restaurant staff are important strategies for minimizing risk. Creating a supportive network of friends, family, and caregivers who are knowledgeable about the allergy can also provide invaluable support.
Our team at New York Food Allergy and Wellness supports and believes that ongoing research and advancements in immunotherapy and other treatments hold promise for the future. As we continue to explore new approaches and preventive measures, there is hope that the burden of peanut allergies will be reduced, and new options will become available for those affected.
Ultimately, living with a peanut allergy requires vigilance, education, and proactive management. By staying informed and taking appropriate precautions, individuals with peanut allergies can navigate their daily lives safely and confidently, reducing the impact of the allergy on their overall well-being. At NYFA, we are creating new standards and a paradigm shift for peanut allergy treatment and we are very excited for the future of all our food allergy patients.

Diagnosis and Testing for Allergies
Diagnosing tree nut and peanut allergies involves a combination of medical history, physical examination, and specific allergy tests. A thorough medical history can provide valuable insights into the patterns and triggers of allergic reactions. This information can help healthcare providers determine whether further testing is necessary and which tests to perform.
Allergy testing typically involves skin prick tests, blood tests, or both. In a skin prick test, a small amount of the allergen is introduced into the skin, usually on the forearm or back, and the area is observed for signs of an allergic reaction, such as redness or swelling. Blood tests, such as the specific IgE test, measure the levels of allergy-related antibodies in the blood. Elevated levels of these antibodies can indicate an allergy to the tested substance.
In some cases, an oral food challenge may be conducted under medical supervision. During this test, the individual consumes small amounts of the suspected allergen in a controlled setting while being closely monitored for any signs of an allergic reaction. This test can provide definitive confirmation of an allergy and help determine the severity of the reaction. It is important to note that oral food challenges should only be performed by experienced healthcare providers in a medical setting equipped to handle severe allergic reactions.
Basophil Activation Test (BAT)
At NYFA, advanced diagnostics may include the Basophil Activation Test (BAT) alongside sIgE blood testing, component testing, and (when appropriate) oral food challenges. BAT is designed to evaluate how basophils, a type of immune cell involved in allergic responses, react when exposed to a suspected allergen in a controlled lab setting. This type of testing can help add clarity when traditional testing results are hard to interpret, especially when a person has never had a clear reaction history.
Many of our new patients come with “food allergy” labels due to positive blood tests or skin tests done at other food allergy institutes without proof of any prior exposure or reactions. By using advanced science, we are de-coding false diagnoses from true food allergies through sIgE tests, component tests, Basophil Activation Tests (BAT), and oral food challenges.
The Power of Desensitization Therapy with NYFA
For over two decades, Dr. Atul Shah has been a pioneer in desensitization therapies for food allergies. His FATE™ Program is specifically designed to help individuals achieve a higher tolerance to allergens, enabling them to live fuller, unrestricted lives. With over 15,000 success stories, this program has been instrumental in changing lives and helping people pursue goals they once thought unattainable.
How the FATE™ Program Works
- Personalized Assessment: Dr. Shah and his team begin with a thorough evaluation of each patient’s allergy severity, medical history, and unique health profile.
- Customized Desensitization Path: A step-by-step approach gradually exposes the patient to controlled amounts of the allergen, building tolerance safely and effectively.
- Ongoing Monitoring & Support: Each patient receives personalized guidance, monitoring, and adjustments to the program as needed to ensure success and safety.
- Real-Life Preparedness: Patients learn how to manage their allergies confidently, even in high-stress, unpredictable situations.
By gradually increasing the body's tolerance to allergens, desensitization can open doors that were once closed, including the possibility of serving in the military.
The Role of NY Food Allergy & Wellness
At NY Food Allergy & Wellness, we focus on clarity, not assumptions. Many patients come in with “food allergy” labels based on testing alone, without a clear reaction history. Our approach combines detailed history with the right testing tools (when needed) to help distinguish false positives from true allergy risk.
Once risk is clarified, we guide patients through practical next steps, whether that means a refined avoidance plan, emergency preparedness, supervised challenges when appropriate, or a structured path toward desensitization support through NYFA’s programs.
NYFA next steps in Manhattan
Visit NYFA’s Manhattan Office
NY Food Allergy & Wellness is located on the Upper East Side at 110 East 60th St., Suite 708, New York, NY 10022. Serving all of Manhattan, the NYC metro area, New Jersey, Connecticut, and patients nationwide, as well as international visitors.
FAQs
The first signs of a peanut allergy often begin soon after exposure and may include an itchy mouth, hives, flushing, swelling of the lips or face, stomach pain, nausea, vomiting, coughing, wheezing, or trouble breathing. Some reactions start with skin symptoms, but not all do, and severe reactions can escalate quickly.
At NYFA, we look at the full picture, including symptom timing, reaction history, and advanced testing when appropriate, because the earliest signs can vary from person to person.
Peanut intolerance and peanut allergy are not the same thing. A true peanut allergy involves the immune system, and yes, some people can develop a peanut allergy later in life even if they previously ate peanuts without a problem. New symptoms after eating peanuts should be evaluated carefully, because not every reaction is a true peanut allergy.
At NYFA, we help determine whether symptoms point to a true peanut allergy, another food issue, or a false-positive label by combining history with targeted testing such as peanut component testing, BAT, and supervised oral food challenges when appropriate.
There is no universal medical diagnosis called a “Level 1 peanut allergy.” Sometimes people use numbered levels informally to describe a past reaction or a lab class on a test result, but those labels do not reliably predict how serious a future reaction may be.
At NYFA, peanut allergy is not judged by a simple level number alone. We focus on your real reaction history, physical findings, peanut component results, Basophil Activation Test data, and when appropriate, supervised oral food challenges to guide next steps.
If you are allergic to peanuts and eat them, you may develop symptoms ranging from mild itching or hives to vomiting, swelling, wheezing, trouble breathing, dizziness, a drop in blood pressure, or anaphylaxis. Because reactions can become severe quickly, suspected anaphylaxis should be treated with epinephrine right away and followed by emergency medical care.
At NYFA, we work to confirm true peanut allergy accurately and then build a personalized plan that may include emergency preparedness, avoidance guidance, and for the right candidates, desensitization options through the FATE™ Program.
Peanut allergy is not considered rare. In the United States, it is one of the most common food allergies, especially in children. Studies suggest that roughly 2.5% of U.S. children and about 1.8% of U.S. adults have convincing peanut allergy.
Because peanut allergy is common and can be serious, NYFA focuses on accurate diagnosis first, so patients are not over-labeled or under-protected.
In the United States, the 9 major food allergens that require labeling are milk, egg, fish, crustacean shellfish, tree nuts, peanuts, wheat, soy, and sesame. These are the major allergens patients and families are most often taught to watch for on packaged food labels.
At NYFA, peanut allergy care is part of a broader food allergy approach, and we also evaluate patients who may be reacting to other major allergens depending on their history, symptoms, and goals.
About Dr. Atul Shah
- Founder of NY Food Allergy & Wellness
- Creator of the FATE™ Program
- 20+ Years of Experience
- 15,000+ Success Stories
- America’s Top Physicians’ Award
- The Patients’ Choice Award
- Most Compassionate Physicians’ Award


